Preview
The prevalence of diabetes is rapidly increasing, fueled by an aging population and climbing incidence of obesity. Given the vast amount of people diagnosed with diabetes, along with many more who are prediabetic and undiagnosed, the market opportunity for innovative treatments and preventative solutions is immense. New technologies for disease management and novel treatment categories are providing hope for effective prevention, management, and treatment of diabetes.
Key Takeaways
- Understanding the Market: Diabetes cases are rising quickly, but patient outcomes are improving, aided by new and innovative treatments.
- Breakthrough Digital Technologies: Companies in the medical device space are leading the transition from finger pricks and insulin injections to continuous monitors and tubeless pumps.
- A New Treatment Paradigm: A new class of treatments known as GLP-1s is helping manage the disease and aid in its prevention.
Understanding the Public Health Emergency
The health care industry, fueled by a growing number of patients, continues to drive innovation in the diabetes space. Diabetes is one of the top leading causes of death worldwide, with 6.7 million adult deaths directly tied to the disease in 2021.1 The number of adults with the illness across the globe is also quickly increasing. Where the figure stood at 151 million individuals in 2000, it now stands at over 537 million patients worldwide.2 The industry forecasts 783 million individuals will have diabetes by 2045, though certain countries are expected to see accelerated prevalence of the illness.3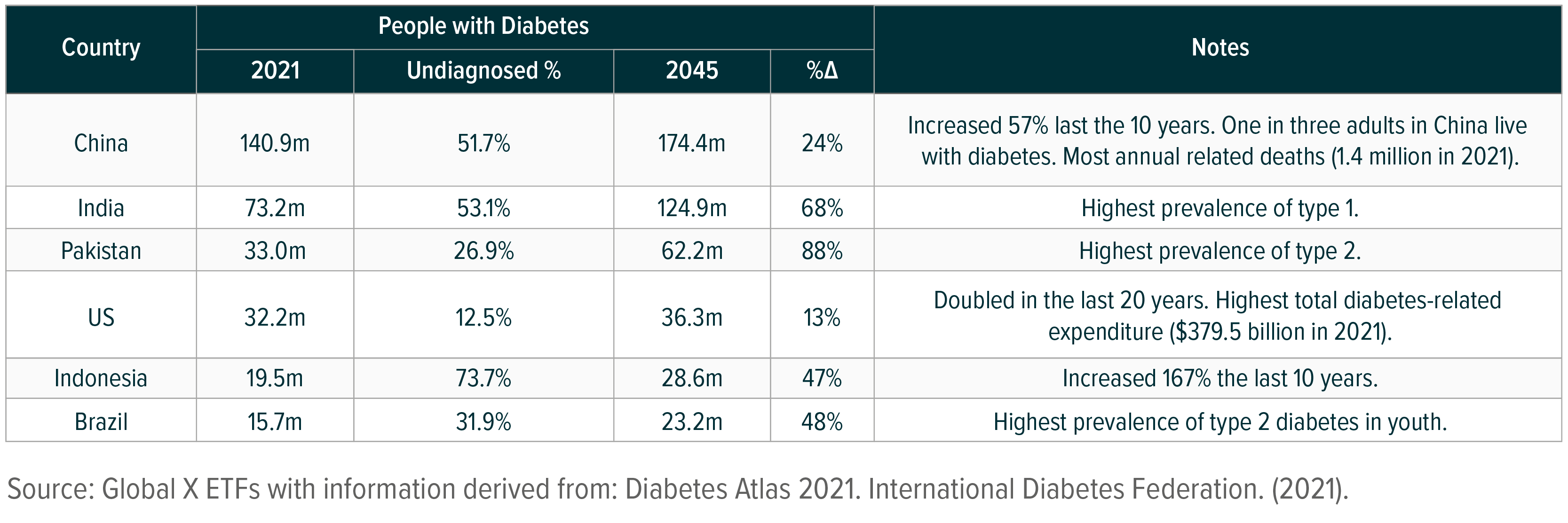
Driven by increased prevalence of diabetes, the illness caused at least $966 billion in health expenditures in 2021, a 316% increase over the last 15 years.4 In the United States, $1 in every $4 in health care costs is spent on caring for individuals with diabetes, with a total estimated $379.5 billion spent in the US on diabetes-related expenses.5, 6 An estimated 48 to 64% of lifetime medical costs for diabetes patients are complications from the illness, such as heart disease and stroke.7
The staggering patient outcomes and economic impact have fueled innovation in the sector, with an array of novel approaches to disease management. Notably, however, treatment of the illness varies depending on the type of diabetes a patient has.
- Type 1 diabetes (T1D) occurs when the pancreas is unable to produce enough insulin and usually develops at an early age. Insulin is a hormone that regulates glucose, or sugar, levels in the blood. T1D cannot be prevented and cannot be reversed. Instead, patients rely on insulin therapy to supplement the body’s own insulin to ensure blood sugar levels stay within a normal range. T1D patients can experience glucose levels that are too high or too low. An estimated 5% of all diabetes cases are type 1.8
- Type 2 diabetes (T2D) occurs due to insulin resistance. This happens when the pancreas pumps out insulin as normal but, over time, cells stop responding to that insulin, causing blood sugar to rise. This type of diabetes usually develops at an older age and is typically compounded by factors like obesity and an inactive lifestyle. If diagnosed early and managed properly, T2D can be reversed. In severe cases, patients rely on diabetes medication or insulin therapy.
Glucose Monitoring: From Finger Pricks to Continuous Data Streams
To determine how well their treatments are working, diabetes patients must measure glucose levels throughout the day. This helps guide the patients on how much insulin their bodies need and when. Keeping track of glucose levels over time also plays a key role in doctor evaluations to manage the condition.
For a long time, patients solely relied on blood glucose monitors (BGMs), which analyze a small amount of blood, usually from finger pricks. This method is up to 95% accurate and can be used four to 10 times a day.9, 10 BGMs also require manual data collection and manual data sharing.
Continuous glucose monitors (CGMs) offer an alternative. These are sensors placed under the skin that measure glucose levels and automatically transfer data to a smart device. The devices measure up to 288 readings a day and automatically collect patients’ data.11 Patients can set up alerts when glucose levels are out of range and can remotely share their data with loved ones or their physician.
CGMs have gained in popularity since first being commercialized in 1999, and new data continue to support the promise of the technology. A recent clinical trial showed a 67% decrease in patient hospitalizations when using a CGM.12
The CGM market is concentrated among three main players: Dexcom, Abbott, and Medtronic. All three companies have recently reported strong revenues, as the industry further embraces the technology. Abbott leads the way in CGM revenue, with an impressive 4.5 million patients utilizing its devices, resulting in estimated revenue of $1,000 per user annually.13 In 2022, Abbott’s diabetes segment generated $4.76 billion in revenue.14 Dexcom, for its part, reported $2.91 billion in sales in 2022, while Medtronic reported $2.3 billion in total diabetes sales in 2022, including its Guardian 4 CGM and MiniMed insulin pump.15

Abbott recently announced plans to grow its Freestyle Libre CGM into a $10 billion product over the next five years, which would represent a 15% compound annual growth rate (CAGR).16 Abbott is also working on a new wearable device that can monitor both glucose and ketone levels to help patients at risk of developing diabetic ketoacidosis, a common complication for Type 1 patients. Dexcom, for its part, expects 2023 revenue to increase 20%, aided by the recent approval of the G7.17 The firm forecasts revenues could reach $3.35 billion to $3.49 billion in 2023.18
Under new guidance by the Centers of Medicare and Medicaid Services (CMS), CGMs are now reimbursed for a wider proportion of diabetes patients, expanding the market opportunity for CGM makers. Specifically, the proposal expands reimbursement to patients who take long-acting insulin, also known as basal insulin, as little as once a day. The new guidance doubles the market opportunity of type 1 and type 2 insulin dependent patients.19 This would be a particularly large win in the type 2 diabetes space, in which CGMs only have about 25% penetration.20
Insulin Pumps: Tubeless Tech Can Drive Further Adoption
The technical enhancements in the care of diabetic patients have also opened a new way to automatically deliver insulin based on a patient’s needs over time. Insulin pumps are small, wearable devices that deliver insulin to diabetes patients and offer an alternative to traditional insulin injections. Insulin pumps are a more consistent and convenient method for insulin delivery, removing patient guess work. When used in combination with a CGM, the pump adjusts insulin levels specifically based on the patient’s blood glucose readings. This is known a closed loop system.
A host of insulin pumps have entered the market in recent years, with Medtronic, Tandem Diabetes, Insulet, and Roche having come out with products that show significant benefit to patients. Currently, an estimated 20-30% of T1D patients utilize them over multiple daily injections (MDIs).21 Given their ease of use, studies have shown insulin pumps can increase the “time in range” (TIR) for diabetic patients by nearly 24%.22 A recent study also showed that T2D patients using Tandem’s t:slim X2 pump, when used in combination with Dexcom’s CGM, spend 3.6 hours a day longer in the target blood glucose range after switching to the closed loop system.23
Technology for insulin pumps is improving rapidly, and newer models offer an improved patient experience via a sleeker, more comfortable design. Traditional insulin pumps usually require a small receiver with a tube that goes under the skin to deliver insulin. Newer models, like Insulet’s Omnipod, offer a tubeless device. These are also known as patch pumps and are small adhesive patches worn directly on the skin. The patch contains all of the mechanisms to seamlessly deliver insulin, without the need for any tubing.
Tubeless devices offer a more convenient system for patients, reducing the risk of the tubing getting dislodged and interrupting insulin delivery. The sleek design is particularly beneficial for active patients and pediatric diabetics. Young patients with diabetes tend to require smaller doses of insulin, have more unpredictable eating habits, engage in more unplanned physical activity, and may struggle to recognize and communicate the need for treatment during episodes of low blood sugar.
Fueled by recent innovation and ongoing adoption of insulin pump technology, pump manufacturers continue to grow their footprint. Insulet reported $1.25 billion in 2022 revenue, representing 20% growth from the prior year, and expects 2023 revenue to grow an additional 14-19%.24 Tandem Diabetes, for its part, reported $801 billion in 2022 revenue.25 Following the 14% growth in 2022, Tandem now projects 10-12% growth in 2023.26 Expected growth from Insulet and Tandem will play a key role in the industry reaching anticipated revenues of $8.3 billion by 2028, up from $4.6 billion in 2021.27
GLP-1s: Offering Hope for Treatment and Prevention of Type 2 Diabetes
A new class of therapies has come to market, improving patient outcomes for type 2 diabetes patients. GLP-1 (glucagon-like peptide 1) stimulates the body to produce more insulin when a patient’s blood sugar levels start to rise, helping manage diabetic symptoms. This treatment category has revolutionized the type 2 diabetes space, with four out of five of the top expected products in T2D in 2028 being GLP-1s.28 To meet demand, both Lilly and Novo look to expand supply capacity of their GLP-1 portfolios, with Eli Lilly looking to double its capacity by the end of 2023.29
This drug category can also help curb hunger, opening its potential use to the obesity market, which is expected to be worth over $50 billion by the end of the decade, up from $2.7 billion today.30 The industry is set to particularly benefit from a broader shift in health care to focus more on causes of illnesses like diabetes and cardiovascular disease rather than treatment of their symptoms. Studies have shown obesity accounts for 80 to 85% of the risk in developing type 2 diabetes, and obese individuals are 80 times more likely to develop the illness than non-obese people.31 Prediabetes patients, for example, could benefit from such treatments. Estimates show that for every type 2 diabetic, a population of 30 million patients in the United States, there are about twice as many prediabetics.32,33
The obesity space is expected to grow at a compound annual growth rate (CAGR) of 37% through 2028, compared to diabetes’ expected 4% CAGR in the same period.34,35
Lily’s Mounjaro showed promising results in its SURMOUNT-1 clinical trial, in which patients achieved average weight reductions of 16%, 21.4%, and 22.5% at 5mg, 10mg, and 15mg doses, respectively.36 The results topped Novo Nordisk’s diabetes drug Ozempic, marketed as Wegovy to obesity patients, which in clinical trials helped patients lose an average 12.4% of their body weight versus placebo.37
The medical community is optimistic about Mounjaro and its potential impact on the obesity market, as its efficacy data compares favorably to conventional surgical approaches. Sleeve gastrectomy surgery and gastric bypass typically result in average weight reductions of 20% and 25-30%, respectively, but come with high risks and cost upwards of $35,000.38 GLP-1s are projected to play a pivotal role in addressing the global obesity epidemic, as global obesity rates have nearly tripled since 1975.39
Conclusion
The landscape for diabetes treatment and prevention has evolved greatly in recent years, with additional breakthroughs likely to follow. Demographic shifts toward an older population, and the ongoing public health problem of obesity, suggest that there is a large market opportunity for companies that can deliver innovative solutions for not just diabetes treatment, but also prevention.
Related ETFs
HEAL – Global X HealthTech ETF
AGNG - Global X Aging Population ETF
SNSR - Global X Internet of Things ETF
Click the fund name above to view current holdings. Holdings are subject to change. Current and future holdings are subject to risk.